Research team: Department of Ophthalmology, Beijing Friendship Hospital, Capital Medical University.
Correspondent: Feng Xue
Foreword: Acute coronary syndrome (ACS) is an acute manifestation of ischemic heart disease. Among cardiovascular diseases, its morbidity and mortality are relatively high. Studies have shown that patients with retinal vascular occlusion have a higher risk of ACS. In order to further explore the relationship between ischemic heart disease and ocular blood flow, Professor Yanling Wang’s team used computer software to reconstruct a three-dimensional model of the ophthalmic artery, quantitatively measure the morphological characteristics of the ophthalmic artery, and obtain the ocular artery’s morphology through numerical simulation of computational fluid dynamics. Hemodynamic information and analysis of the correlation between the characteristics of the ophthalmic artery and the clinical parameters of ACS provide a new perspective for exploring the relationship between ischemic heart disease and ocular signs.
A few days ago, the team of Professor Yanling Wang from the Department of Ophthalmology, Beijing Friendship Hospital, Capital Medical University, published a paper "Ophthalmic Artery Morphological and Hemodynamic Features in Acute Coronary Syndrome" in the well-known journal "Investigative Ophthalmology & Visual Science" for basic research in the field of ophthalmology. The research focused on acute coronary artery synthesis. The morphological and hemodynamic changes of the ophthalmic artery in patients with acute coronary syndrome (ACS), and the correlation between the characteristics of the ophthalmic artery and the clinical parameters of ACS. This cross-sectional study included 31 ACS patients and 10 healthy controls. The ACS patient group was divided into ST-segment elevation myocardial infarction group (n=10) and non-ST-segment elevation myocardial infarction group (n =10) and unstable angina group (n=11). The three-dimensional model of the ophthalmic artery was reconstructed by computer software, the morphological characteristics of the ophthalmic artery were quantitatively measured, and the hemodynamic information of the ophthalmic artery was obtained through numerical simulation of computational fluid dynamics.
The study reconstructed 41 ophthalmic artery models. Hemodynamic simulation data showed that compared with the control group, the blood flow velocity at the beginning of the ophthalmic artery in ACS patients was significantly reduced (average velocity, 0.046 vs 0.147 m/s; P <0.001). No difference was observed in the morphological data of the ophthalmic artery. In addition, it was found that there were differences in the ophthalmic artery blood flow between the ACS group and the normal control group. And similar differences were observed between the ACS subgroup and the control group. Ophthalmic artery blood flow velocity is negatively correlated with body mass index, abdominal circumference, left ventricular ejection fraction and triglycerides, and positively correlated with early to late transventricular flow velocity, N-terminal pro-brain natriuretic peptide, serum creatinine and potassium. Research conclusions: The blood flow velocity at the beginning of the ophthalmic artery in ACS patients is slow, and the shape and mass flow of the ophthalmic artery do not change significantly. The characteristics of the ophthalmic artery are related to the clinical parameters related to ACS.
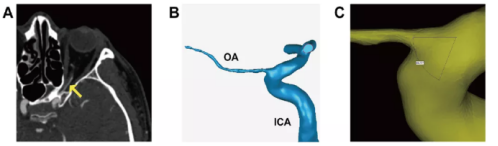
Figure 1 Computer software reconstruction of the three-dimensional model of the ophthalmic artery and an example of morphological data measurement
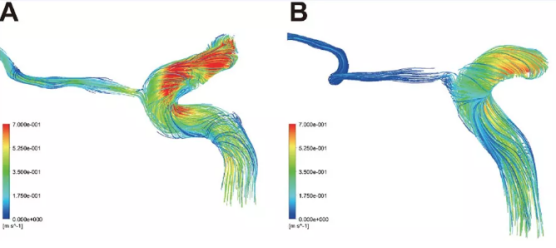
Figure 2 Ocular artery streamline diagram of the representative cases of the normal control group and the ACS group
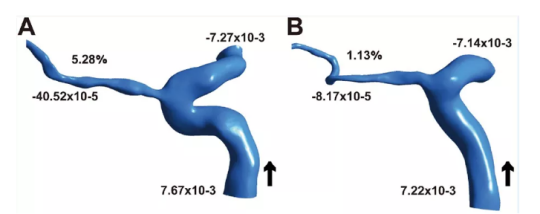
Figure 3 The proportion of ophthalmic artery flow between the normal control group and the representative model of the ACS group
Paper link:https://doi.org/10.1167/iovs.62.14.7

Professor Wang Yanling
Wang Yanling, the corresponding author of this article, is currently the director of the Department of Ophthalmology, the second-level chief physician, doctor of medicine, professor, and doctoral supervisor of Beijing Friendship Hospital affiliated to Capital Medical University. He graduated from Shandong Medical University in 1988. In 1996, he was dispatched to Japan's Kansai Medical University to study ophthalmology. Deputy Dean of the School of Ophthalmology, Capital Medical University, Member of the Neuro-ophthalmology Group of the Ophthalmology Branch of the Chinese Medical Association, Member of the Fundus Ophthalmology Group of the Ophthalmology Branch of the Chinese Medical Doctor Association, Deputy Director of the Ophthalmology Branch of the Beijing Medical Association, Deputy Director of the Ophthalmology Branch of the Beijing Society of Integrative Medicine Member, editorial board member of Chinese Journal of Ophthalmology and Chinese Journal of Fundus Diseases.
Professor Wang Yanling is mainly engaged in vitreoretinal surgery for macular diseases such as high myopia macular split, and has extensive experience in formulating individualized surgical treatment plans for patients with macular diseases. Long-term commitment to clinical and basic research on the interdisciplinary of ophthalmology and systemic diseases, especially in-depth research on the correlation between cardiovascular and cerebrovascular diseases and retinal vascular diseases, as well as precise diagnosis and treatment. In 2017, the organization took the lead in establishing the Ophthalmology and Vascular Disease Multidisciplinary Diagnosis and Treatment Center of the School of Ophthalmology, Capital Medical University, led the team to form a characteristic discipline of ischemic eye disease, and published a series of high-quality articles. Won the 2017 "Top Ten Research Highlights of Neuro-ophthalmology in China", presided over a number of projects including the National Natural Science Foundation, published more than 90 ophthalmology academic papers, included more than 30 papers in SCI, and had 3 utility model patents.

Wang Jialin Attending Physician
Wang Jialin, the co-corresponding author of this article, is an attending physician in the Department of Ophthalmology, Beijing Friendship Hospital, Capital Medical University, and a doctor of medicine. Young member of the Beijing Ophthalmology Branch of Integrated Traditional Chinese and Western Medicine, and young member of the Macular Science Group of the Ophthalmology Committee of the Cross-Strait Medical and Health Exchange Association. Mainly engaged in clinical and basic research of ocular fundus diseases, especially in-depth research in cross-disciplines such as ischemic ophthalmopathy, ocular and systemic diseases. Presided over a number of topics such as innovative talents of the Beijing Municipal Hospital Administration. As the first author or corresponding author, he has published more than 30 ophthalmology academic papers at home and abroad, and more than 10 papers have been included in SCI journals such as "Investigative Ophthalmology & Visual Science", "Eye", "Graefe's Archive for Clinical and Experimental Ophthalmology". He has given many speeches at conferences such as APVRS, China-Japan-Korea Ophthalmology and National Ophthalmology Annual Meeting.

Master Wu Lanting
Wu Lanting, the first author of this article, a long-term master of clinical medicine in Capital Medical University, a master student in Ophthalmology, Beijing Friendship Hospital, Capital Medical University