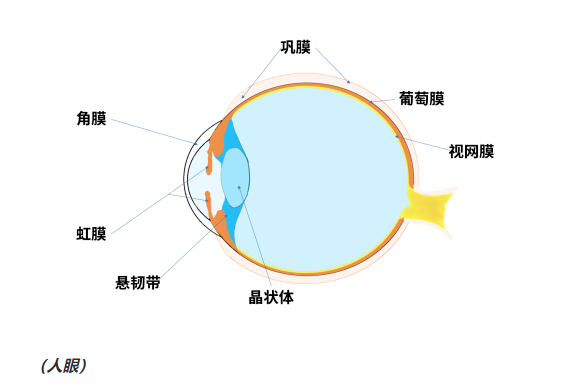
Cornea is a transparent dome shaped membrane in front of the eyeball. You can simply understand it as "the first lens of human eye camera". It has powerful focusing function, including transmitting light, refracting light and preventing foreign bodies from entering.
However, as one of the most superficial and important refractive stroma, the cornea is extremely vulnerable to various external injuries. When the cornea becomes turbid, cannot correctly refract light or has holes damaged due to inflammatory infection, trauma or genetic diseases, the vision will be seriously damaged, even disabled and blind.
With the continuous improvement of corneal transplantation skills, some patients can reconstruct visual function through corneal transplantation. However, there are still many patients with serious ocular surface damage, corneal scar formation and a large number of neovascularization on the corneal surface, which makes the traditional corneal transplantation very easy to reject.
Moreover, due to the lack of corneal donors, the restriction of economic conditions and the risk of surgery, there are only about 3000 to 5000 cases of corneal transplantation in China every year.
Some patients give up the hope of vision restoration because of pannus on the corneal surface after multiple corneal transplantation rejection.
Today, mikh can tell you loudly: those patients with binocular corneal blindness who are difficult to succeed in corneal transplantation can believe in light again!

The success rate of penetrating keratoplasty is more than 90%, but for severe corneal scar and vascularization caused by severe acid-base chemical burns, irrecoverable eye face or conjunctival sac dysfunction, such as complete atresia symblepharon, Stevens Johnson syndrome (SJS) eye scar pemphigus (OCP), and multiple corneal transplantation failures with severe graft bed neovascularization, The success rate of penetrating keratoplasty is almost zero.
Artificial corneal implantation is the only hope for these patients to recover their eyesight, and mikh artificial cornea is the last hope of these patients!
A cold knowledge: before artificial cornea, the first solution that scientists thought of was animal cornea, of which pig cornea is the most commonly used, because the morphological similarity between pig cornea and human cornea can reach 94%.

However, because porcine cornea is a "xenograft", the problem of immune rejection is very serious. At the same time, how to remove various pathogenic bacteria, parasites and other microorganisms carried on pig cornea is still a problem to be studied.
Compared with animal cornea, artificial cornea may be a better solution. However, in recent years, although the artificial cornea technology has been developed, it is still faced with problems such as "how to maintain the best postoperative corrected vision and deal with various complications".
For example, AlphaCor artificial cornea has frightening complications. The thinning and dissolution of anterior corneal stroma and the formation of artificial corneal fiber exudative membrane (RPM) may lead to refractory glaucoma and even the excretion of artificial cornea in some patients.
Rpm is the proliferation of fibrous vascular tissue on the inner surface of artificial cornea, which can block the optical area. It is one of the main reasons for the decline of visual acuity after operation. The incidence of RPM in Boston artificial cornea is as high as 27% ~ 65%. In addition, there may be persistent upper skin defect, aseptic vitreitis, endophthalmitis and retinal detachment after Boston artificial cornea operation. Their prevention and treatment also directly affect the correction of visual function of postoperative patients.
The Michaelis artificial cornea is made of artificial materials without donor cornea, which not only saves part of the cost, but also avoids the rejection reaction.
Mikh artificial cornea is an artificial cornea with independent intellectual property rights developed by mikh medical. The central optical part is connected with the titanium support through threads. The processing precision is very high. The watertight combination between the mirror column and the bracket screwed in place can prevent low intraocular pressure caused by water leakage and reduce the chance of intraocular infection.
It is worth mentioning that MIH artificial cornea adopts staged surgical implantation. Through intraocular perfusion and small corneal opening, serious intraoperative complications such as Boston artificial cornea and AlphaCor artificial cornea, such as expulsion bleeding and water leakage, can be avoided to the greatest extent.
In addition, the possibility of tissue lysis is also reduced by the method of Michaelis artificial cornea surgery. Compared with the allogeneic corneal carrier in Boston artificial cornea, it mainly depends on the aqueous humor to provide nutrition and maintain its epithelial integrity. During the operation, the Michaelis artificial cornea promotes the vascularization of the ocular surface as soon as possible through the covering of conjunctiva or labial mucosa, so as to maintain the nutritional supply of the anterior lamellar tissue, so as to reduce tissue dissolution.

At the same time, scholars have found that rpm is related to postoperative inflammation and artificial corneal displacement. Therefore, in the process of operation, we can avoid the displacement of artificial cornea by removing relevant useless tissues, appropriately increasing the length of artificial corneal column, cartilage reinforcement and ocular muscle truncation, so as to reduce or even avoid the occurrence of RPM.
Facts have proved that this method can indeed solve the problem of RPM. Relevant clinical data showed that the patient had rpm. After surgical resection, there was no recurrence during follow-up.
Due to the immaturity of some product technologies and the incompleteness of operation methods, there is no "blooming flowers" in the field of artificial cornea for the time being. However, with the continuous deepening of research and the continuous improvement of technology, it is believed that in the future, there will be more artificial corneas that can help more and more patients with corneal blindness see the light again.
References:
① Animal experiment and clinical study of mikh domestic artificial cornea Meng Xiaoli
② Application of micof artificial cornea in patients with corneal blindness Yu Jifeng