According to the data reported by the World Health Organization, corneal disease is one of the most important blinding eye diseases. It is the second general blinding eye disease after cataract in developing countries, and it is also the first pathogenic factor of enucleation.
There are about 4million patients with corneal blindness in China. 85% of corneal blindness comes from infectious keratopathy, and more than 100000 new cases of infectious keratopathy cause blindness every year.
Corneal transplantation is a surgical method that uses allogeneic normal transparent corneal tissue to replace the unhealthy corneal tissue with cloudy lesions, so as to control the progression of lesions and improve visual function.
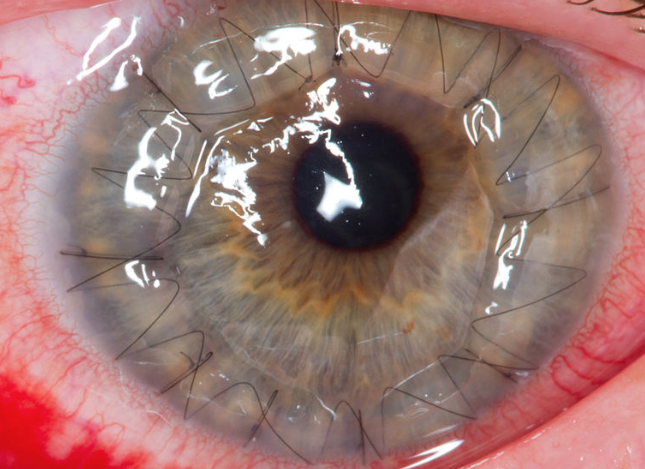
According to the scope, degree and nature of corneal lesions, componential keratoplasty has been widely carried out in clinic. More than 80% of patients with corneal blindness can be restored by conventional donor corneal transplantation.
However, the key to corneal transplantation is to have healthy corneal donor materials. In China, the prevention and treatment of corneal diseases are limited by many conditions: grass-roots doctors lack sufficient professional knowledge of cornea, the misuse and abuse of drugs make patients unable to receive early standardized diagnosis and treatment, and the source of corneal donors is seriously scarce, which limits the implementation of corneal transplantation.
In addition, about 15% of the clinical patients with corneal blindness are high-risk corneal transplant patients with severe eye burns (chemical burns, thermal burns), multiple failures of routine corneal transplantation, substantial dry eyes, severe neurotrophic keratopathy, ocular pemphigoid, Stevens Johnson syndrome and cicatricial keratoconjunctival diseases. Routine corneal transplantation is difficult to succeed, and artificial corneal transplantation is the only hope for vision restoration.
At present, patients with the following four types of eye diseases can consider artificial corneal transplantation if corneal transplantation fails.
① Patients with corneal diseases caused by trauma and acid and alkali chemical burns, severe corneal scar, corneal vascularized corneal leukoplakia, and eyelid atresia in the late stage of the disease
② Corneal blindness patients with corneal transplantation failure
③ Serious autoimmune diseases (such as Stevens Johnson syndrome and cicatricial pemphigoid), corneal blindness caused by end-stage dry eye, corneal limbal lysis caused by corneal tissue dissolution and destruction, corneal dystrophy and degeneration
④ Patients with bilateral corneal blindness who are difficult to succeed in corneal transplantation
Due to the lack of commercial artificial cornea products for clinical use in China in the past, this part of corneal blindness has almost become a "terminal disease" of ophthalmic rehabilitation.
But now, with the completion of clinical trials and registration evaluation of Microk, domestic artificial cornea will bring opportunities for end-stage corneal blindness in China.

Micof is composed of transparent medical PMMA optical lens column and titanium stent, which can be adjusted and selected according to the patient's ocular surface conditions.
Compared with the Boston artificial cornea in the world, the biggest difference of the Micof is that it does not need a donor cornea, which avoids the rejection reaction after surgery and shortens the time for patients to regain vision.
Micof is suitable for bilateral corneal blindness, mainly for severe keratoconjunctival scar vascularization caused by eye burns or explosive injuries. Eyelid atresia, severe Steven Johnson syndrome, cicatricial pemphigoid, end-stage symblepharon or severe eyelid deformity.
In addition, in order to ensure the safety of the operation, Michel keratoplasty was divided into two stages.
The artificial corneal scaffold was implanted in the first stage, and the optical lens column was installed in the second stage, which was implemented 3 months after the first stage operation. Patients should be reexamined on the first day, one week, and two to three weeks after surgery. After that, recheck once a month and 4 times a year later to record vision, etc.